Good question that gets to the science of INDY Neurofeedback and what it can tell us about how our brains operate.
Humans have five different types of electrical patterns or “brainwaves.” The five brainwaves are generally listed in order of highest frequency to lowest and include: Gamma, Beta, Alpha, Theta, and Delta waves. They can be seen with the help of a qEEG (quantitative electroencephalograph), sometimes called brain mapping.
At INDY Neurofeedback, we know that every brainwave we map has a different and vital purpose. Research has demonstrated that there is an accepted normal pattern of brainwave activity. Each wave helps us cope with different types of situations – from processing and learning new information to helping us calm down after a lot of stress.
If one of the five types of brainwaves is either overproduced and/or under produced in our brain, it can compromise our daily lives. No single brainwave is “better” or more “optimal” than the others.
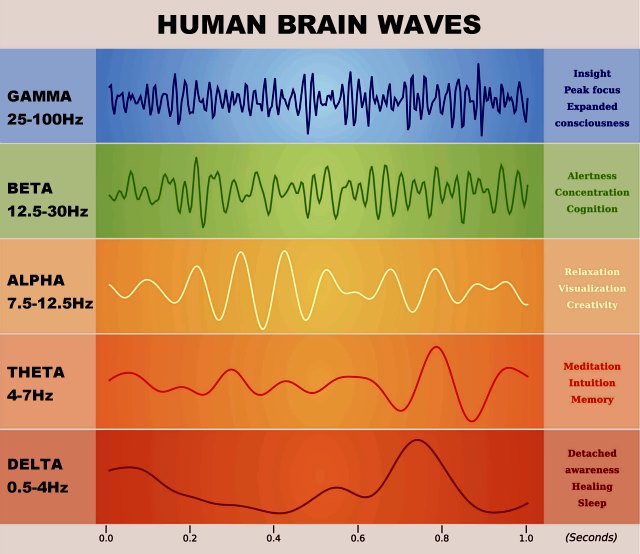
Here’s how our brainwaves function
While in a wakeful state, a qEEG will display all five types of brainwaves at the same time. This brain map allows us to see brainwave imbalances. The goal of neurofeedback is to transform an unhealthy, dysregulated brainwave imbalance into a normal, healthy, organized pattern. By doing this, the brain becomes more stable and is able to operate optimally and efficiently.
For example, those with ADD/ADHD have slower brainwaves than that of the rest of the population. They produce slow Theta waves when they should be producing fast Beta waves. The ADD/ADHD person compensates for the increased Theta production with hyperactivity. During sleep, clients usually have combinations of the slower frequencies, but during deep REM (rapid-eye movement) sleep, more Gamma activity is present.
- Gamma waves are involved in higher processing tasks. They are important for learning, perception, memory, and information processing. Individuals who have learning disabilities tend to have lower Gamma activity than average.
Frequency range: 40 Hz to 100 Hz (Highest)
Too much: Anxiety, high arousal, stress
Too little: ADHD, depression, learning disabilities
Optimal: Binding senses, cognition, information processing, learning, perception, REM sleep
- Beta waves are high frequency, low amplitude brain waves that are occur while we are awake. They are involved in conscious thought, logical thinking, and tend to have a stimulating affect. Having the right amount of Beta waves allows us to focus and complete school or work-based tasks easily. Having too much Beta may lead to us experiencing excessive stress and/or anxiety. The higher beta frequencies are associated with high levels of arousal.
Frequency range: 12 Hz to 40 Hz (High)
Too much: Adrenaline, anxiety, high arousal, inability to relax, stress
Too little: ADHD, daydreaming, depression, poor cognition
Optimal: Conscious focus, memory, problem solving
- Alpha waves bridges the gap between our conscious thinking and our subconscious mind. It helps us calm down and promotes feelings of deep relaxation. If we become stressed, a phenomenon called “Alpha blocking” may occur which involves excessive beta activity and very little alpha. Essentially the Beta waves “block” out the production of alpha because we become too aroused.
Frequency range: 8 Hz to 12 Hz (Moderate)
Too much: Daydreaming, inability to focus, too relaxed
Too little: Anxiety, high stress, insomnia, OCD
Optimal: Relaxation
- Theta waves are involved in daydreaming and sleep. They are responsible for us experiencing deep and sometimes raw emotions. Too much Theta activity may make people prone to bouts of depression and may make them “highly suggestible.” Theta helps improve intuition, creativity, and is also involved in restorative sleep.
Frequency range: 4 Hz to 8 Hz (Slow)
Too much: ADHD, depression, hyperactivity, impulsivity, inattentiveness
Too little: Anxiety, poor emotional awareness, stress
Optimal: Creativity, emotional connection, intuition, relaxation
- Delta waves are the slowest human brain waves found most often in infants and young children. As we age, we tend to produce less. Delta waves are associated with the deepest levels of relaxation and restorative, healing sleep and unconscious bodily functions such as regulating heart beat and digestion.
Frequency range: 0 Hz to 4 Hz (Slowest)
Too much: Brain injuries, learning problems, inability to think, severe ADHD
Too little: Inability to rejuvenate body, inability to revitalize the brain, poor sleep
Optimal: Immune system, natural healing, restorative / deep sleep
Understanding how each of these brainwaves work together is an important and fascinating part of what we do at INDY Neurofeedback. We work with clients to help them understand the unique individual strengths and weaknesses of their brains, and with highly specialized training, work to retrain their brains for more optimal functioning. Neurofeedback is a non-invasive approach to optimal brain functioning and improved health.
To get your questions answered about your brainwave functioning, consider scheduling a qEEG with us.


 There’s been some recent buzz on the Internet about introverts. According to self-reporting, introverts seem to cope with quarantine conditions better than their more extroverted friends. If you’ve shared in similar discussions, you might wonder if you tend toward introversion or extroversion. Because, well — is anyone exclusively just one type of personality?
There’s been some recent buzz on the Internet about introverts. According to self-reporting, introverts seem to cope with quarantine conditions better than their more extroverted friends. If you’ve shared in similar discussions, you might wonder if you tend toward introversion or extroversion. Because, well — is anyone exclusively just one type of personality?
 At INDY Neurofeedback, a frequently asked question is, “What is neurofeedback?” And secondly, “Is this the same as biofeedback?”
At INDY Neurofeedback, a frequently asked question is, “What is neurofeedback?” And secondly, “Is this the same as biofeedback?”
 Would you have trouble memorizing and repeating back ten un-related words? How easily do you absorb driving directions before using them?
Would you have trouble memorizing and repeating back ten un-related words? How easily do you absorb driving directions before using them?
 Did you know that the rhythm of your breathing influences brain activity such as memory recall and emotional judgment?
Did you know that the rhythm of your breathing influences brain activity such as memory recall and emotional judgment? The simplest answer is that we don’t know for sure. But in recent medical studies, essential oils and aromatherapy do seem to have a positive effect upon those with brain disorders such as dementia and Alzheimer’s disease.
The simplest answer is that we don’t know for sure. But in recent medical studies, essential oils and aromatherapy do seem to have a positive effect upon those with brain disorders such as dementia and Alzheimer’s disease. Quite a few people think so.
Quite a few people think so.